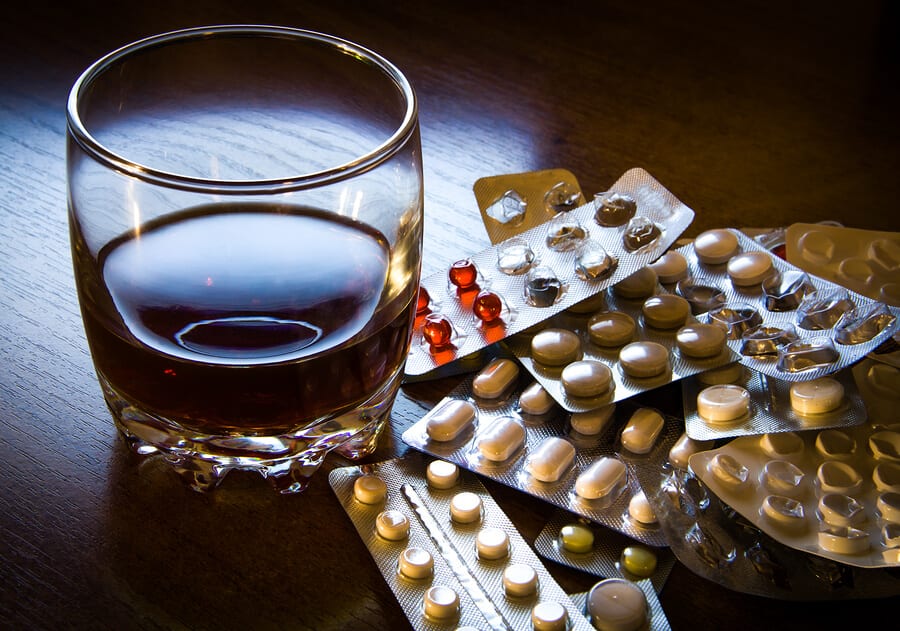
Depressants and Abuse – Central nervous system (CNS) depressants are substances that reduce activity in the brain and body. Prescription depressants are used for the treatment of a variety of conditions, such as insomnia, anxiety, seizures, and muscle tension.
When misused, however, these drugs can have a negative impact on the body, leading to serious complications, overdose, and even death. Common depressants include alcohol, benzodiazepines, opioids, muscle relaxers, hypnotics, and sedatives.
Commonly Abused Depressants
Alcohol
Alcohol is by far the most frequently used depressant, though it is sometimes mistaken for a stimulant due to the euphoria it initially induces during early levels of intoxication. While alcohol is legal to consume in most areas of the United States for adults over age 21, it is often abused, and those who use alcohol consistently and in large amounts run the risk of addiction and acute alcohol poisoning.
Nearly 90% of adults aged 18 or older report having consumed alcohol at some point in their lives. A further one-fourth of this group have engaged in binge drinking—a pattern of alcohol abuse that increases the risk of adverse effects and alcoholism later on in life.
According to the National Institute on Alcohol Abuse and Alcoholism (NIAAA), negative effects of chronic, excessive alcohol use may include the following:
- Weakened heart muscles
- Irregular heartbeat
- Stroke
- High blood pressure
- Alcoholic hepatitis
- Liver cirrhosis
- Pancreatitis
- Weakened immune system
- Disorientation
- Vision impairment
- Injuries (e.g., falls)
- Anxiety and depression
Chronic alcohol use also increases the risk of cancers of the mouth, throat, esophagus, breast, liver, and colon.
Opiates and Opioids
Opiates and opioids belong to a class of drugs that include both prescription narcotics and illicit substances such as heroin. Due to their highly addictive properties, they are frequently abused for their euphoric and pain-reducing effects. While technically classified as painkillers, opioids and opiates also have depressant effects that can be profound if abused, especially when in combination with other depressants such as alcohol.
Health complications related to opioid use include, but are not limited to the following:
- Heart palpitations
- Sweating and chills
- Nausea
- Vomiting
- Hypersensitivity to stimuli
- Confusion
While many other depressants, including alcohol and benzodiazepines, are relatively unlikely to cause a lethal overdose, powerful opioids such as heroin and fentanyl can result in death in just minutes. As noted, opioids are far more dangerous when used in conjunction with other CNS depressants such as benzos, alcohol, and sedatives.
Barbiturates
Barbiturates have been used for a variety of purposes, such as anesthesia, seizure management, and pain reduction. They are also sometimes employed for the treatment of alcohol withdrawal symptoms. Like many other depressants, barbiturates have a high potential for addiction if abused.
Side effects of excessive barbiturate use include the following:
- Heavy sedation
- Heart palpitations
- Psychological and physiological dependency
- Accidental overdose and death
Problematic habits of barbiturate use can form in a short amount of time. Moreover, these drugs are involved in an estimated 1500 emergency department visits each year. By some estimates, barbiturates may currently be linked to as many as one-third of the drug overdose fatalities in the U.S, though this is rarely discussed in popular media.
Benzodiazepines
Benzos are anti-anxiety medications prescribed for the treatment of conditions such as anxiety and panic disorder, insomnia, and sometimes seizures or depression. Benzos, however, have a high potential for abuse and dependence.
Side effects of benzodiazepine misuse may include the following:
- Sedation
- Confusion
- Depression
- Irritability
- Aggression
- Dizziness
- Unsteadiness
- Weakness
- Loss of orientation
- Headache
- Sleep disturbances
- Impaired memory
Benzo use is rarely fatal if they are abused on their own, but when taken in combination with other CNS depressants such as alcohol or opioids, the risk of a lethal overdose increases exponentially. In fact, benzos are involved in a significant percentage of drug overdose fatalities each year, particularly those classified as combined drug intoxication by medical examiners.
Other Depressants
There are several other drugs classified as depressants that are less likely to be abused but have the potential to adversely interact with other CNS depressants. As a result, depressants should only be used with other psychoactive substances if directed by a doctor.
Other depressants include the following:
- Antihistamines – used to mitigate allergic reactions, inflammation, and in some cases also work as mild anti-anxiety agents.
- Muscle Relaxers – used to relieve strain and tension on the muscles due to surgery, injury, or other debilitating conditions.
- Anti-psychotics – used to treat hyperactive moods during manic episodes or symptoms of psychosis and Tourette’s syndrome.
- Alpha and beta blockers – used to treat Raynaud’s disease, high blood pressure, and anxiety disorders.
Treatment for Addiction to Depressants
Harmony Recovery Center offers a comprehensive approach to addiction treatment that includes psychotherapy, individual, group and family counseling, 12-step programs. Our center also employs holistic health and wellness approaches such as yoga, meditation, and art or music therapy. After intensive treatment has been completed, patients can benefit from our aftercare planning services and alumni activities that foster ongoing community support and continued recovery.
If you suspect that you or someone you love is addicted to depressants, please contact us today to discuss treatment options. Discover how we help people free themselves from the shackles of addiction so they can begin to experience the healthy and satisfying lives they deserve!
READ THIS NEXT: Reasons to Call an Interventionist